Broken heart syndrome remains a mysterious, rare condition that only now is slowly being elucidated. It was first identified by a Japanese researcher who named it Takotsubo cardiomyopathy in 1990. This cardiomyopathy is very different from a heart attack and can be misdiagnosed until specific tests reveal its intrinsic characteristics.
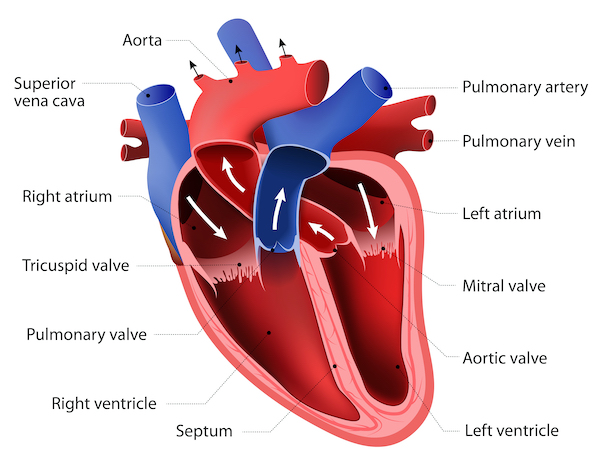
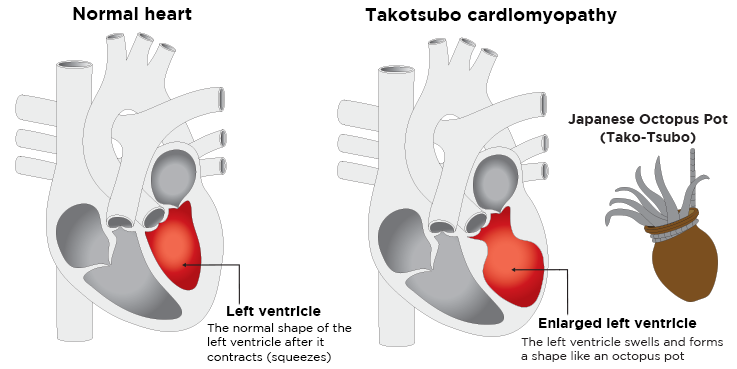
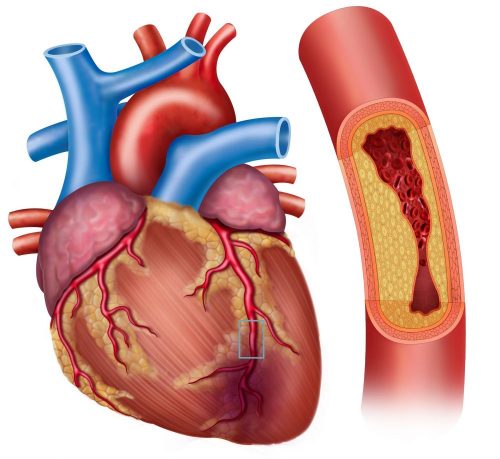
While a heart attack is caused by the blockage of a coronary artery, the arteries in a broken heart syndrome patient are clear. What is visible in a radiological scan (coronary angiogram) though is the unusual ballooning of the left ventricle, the heart’s main pumping chamber. For its similar morphology, the researcher called it Takotsubo, in reference to the pot-trap used to catch octopuses in Japan.
What also differs from a heart attack is the absence of the typical increase in blood biomarkers of heart damage.
Beside Takotsubo cardiomyopathy, this condition is also called stress cardiomyopathy or apical ballooning syndrome. Regarding the clinical management, procedures that are routinely used to treat a heart attack, such as surgery or balloon angioplasty and stent placement, do not bring any advantage in treating broken heart syndrome, which is mostly reversible over the course of a few days, or up to four weeks to normalise heart function.
What is the cause of a broken heart syndrome?
Broken heart syndrome is caused by a sudden, traumatic situation or extreme emotion that produces a huge surge of stress hormones like adrenaline, so strong that it confounds areas of the heart muscles, preventing them from efficiently contracting and pumping blood out to the vessels. The accumulation of blood in the left ventricle leads to the formation of a bulging balloon due to the increased internal pressure in the heart cavity. The heart pumping function is consequently disrupted, with other areas of the heart attempting to compensate with forceful contractions.
When this happens, people experience chest pain, difficulty in breathing, collapse and in rare cases, heart failure, which has been shown in 20% of patients with broken heart syndrome. In sporadic circumstances, patients may experience abnormal heart rhythm, obstruction of blood flow in the left ventricle and even rupture of the ventricle wall. Naturally, at presentation the first thought is of an ongoing heart attack. Of note, broken heart syndrome can occur in healthy people!
Potential triggers of broken heart syndrome are:
- Death of a loved one (often elderly spouses dying within a short time from one another)
- Worrisome medical diagnosis
- Domestic abuse
- Losing / winning — the lottery
- Strong arguments
- Surprise party
- Intense fear
- Job loss or financial difficulty
- Divorce
- Physical stressors: traumatic/road traffic accidents, asthma attacks, COVID-19 infection, bone fracture and major surgery
The Mayo clinic also reports prescription drugs and illicit substances among these causes, which can induce the production of stress hormones:
- Epinephrine (EpiPen) to treat severe allergic reactions or an asthma attack
- Duloxetine to treat nerve problems in people with diabetes, or depression
- Venlafaxine, a treatment for depression
- Levothyroxine, a drug given for thyroid dysfunction
- Unprescribed or illegal stimulants, such as methamphetamine and cocaine

Women are more likely to suffer from broken heart syndrome
Although rare overall, broken heart syndrome mostly affects postmenopausal women. Other risk factors include a history of head injury or epilepsy, as well as anxiety and depression. Generally, there are no lasting effects following a broken heart syndrome, although in rare cases it can be fatal.
The complications arising from the broken heart dysfunction involve the accumulation of fluid in the lungs (lung oedema), low blood pressure (hypotension), irregular heartbeat or severe heart failure. A broken heart syndrome does not usually have recidivism, but it can occur again in 10-15% of the patients. Therefore, it is useful to manage stress and anxiety with a variety of means that have become popular such as yoga and meditation. Pharmacological treatment with beta-blockers is also recommended to reduce the potential damage to the heart should another episode occur. Diuretics can help in case of lung oedema and possibly blood thinners like aspirin with proven presence of arterial plaques (atherosclerosis).
How is broken heart syndrome diagnosed?
The plan to reach a diagnosis for a broken heart syndrome is similar to that used after a heart infarct and is key to exclude an ongoing heart attack.
- Medical history of heart disease, specific stressors and physical examination
- Electrocardiogram (ECG) to monitor the electrical impulse patterns of the heart, which can be abnormal after a broken heart syndrome
- Echocardiogram (ultrasound of the heart) to see possible changes in the ventricle anatomy and presence of ballooning
- Blood tests for cardiac reference enzymes used as markers for heart damage (small, early increase possible)
- Cardiac MRI for a more detailed visualisation of the heart
- Coronary angiogram to identify any abnormalities and occlusions of the coronary arteries of the heart
Research insights: The heart-brain connection
The brain response to stress is governed by neural structures of the limbic system, including the amygdala. Exaggerated neural activity in these brain regions, caused by chronic stress, increases the response of the sympathetic nervous system, potentially contributing to broken heart syndrome.
A recent study has demonstrated a major role for the brain-heart connection underlying the broken heart syndrome. Using functional MRI scans (to visualise brain neural activity rather than brain anatomy only), the researchers have identified altered neural connectivity in those brain limbic regions, associated with stress in individuals who later developed broken heart syndrome.
Out of 104 patients, 41 subsequently developed the heart condition. This means that these patients had a much higher metabolic activity in these brain regions consistent with a heightened response to stress. This altered brain connection can be interpreted to be a predictor of broken heart syndrome in the event of stressful circumstances.
In addition, this stress related brain activity was also associated with altered function of the bone marrow, which produces all blood and immune cells. With such changes in cells carrying oxygen and cells involved in the immune response, the cardio-vascular system may be significantly affected.
Research from the University Hospital Zurich showed that compared to normal subjects, 15 patients with broken heart syndrome presented a disconnection between the brain regions controlling emotions and automatic body responses, such as the heartbeat. The author stated: “Emotions are processed in the brain so it is conceivable that the disease originates in the brain with top-down influences on the heart.”
What is the relevance of broken heart syndrome in the medico-legal space?
Christine Mercer
Lex Medicus Queensland State & Legal Manager
Interestingly, broken heart syndrome was recognised as an accepted condition in a workplace injury claim involving psychological injury. The broken heart syndrome was recognised as being linked to an original psychological workplace injury and thereby met the requisite legal threshold of being an accepted workplace injury for which compensation was being sought.
Below you can find a relevant compensation case of an employee affected by Takotsubo cardiomyopathy.
Galea v Secretary, Department of Communities and Justice [2020] NSWWCC 253
This is a workers’ compensation case with an initial accepted Workcover claim, whereby the female disability support worker suffered harassment, physical assault and bullying by her co-workers and a patient, leading to the development of a psychological injury in the form of PTSD and an adjustment disorder.
This psychological injury arose as a result of what was described as “the appalling conduct” of a colleague of Ms Galea, who had spread saliva from a disabled patient infected with hepatitis onto food Ms Galea later ate. After reporting this incident to her employer, Ms Galea was met with hostility and was verbally harassed by him. Ms Galea had also been involved in a work-related incident where she was trapped in a bus with a disabled patient, who physically abused her for an hour. Ms Galea left her employment, and the psychiatric conditions were accepted as being a result of the recognised workplace injury.
It is a further incident and new injury that is the subject of the case and Commission hearing. A year after Ms Galea had left the employment, she met an ex-colleague, who was involved in the original incident, in a shopping centre. The stress caused by that encounter was so strong that she believed she was having a heart attack and on admission to hospital was diagnosed with Takotsubo cardiomyopathy.
The question in this case, was whether the development of this heart condition was directly linked to the prior workplace injury, thereby attracting further compensation for injury.
Of note were the comments of the treating doctors and the comments of the Commission, who all recognised the significance of the heart condition, the Commission stating: “The medical evidence supports a finding that the applicant’s TCM, otherwise known as ‘broken heart syndrome’, is a cardiac condition secondary to psychological factors, in particular extreme emotion.”
The expert cardiologist commented: “In my opinion, her pre-existing psychological condition (PTSD in relation to bullying and harassment at work) was a key factor in provoking anxiety which subsequently led to her Takotsubo cardiomyopathy.”
Further expert evidence on the causative link stated: “She has a condition called Takotsubo Cardiomyopathy which is well-known to be emotionally brought on and it does not occur spontaneously. Therefore, she had a significantly greater risk of suffering this cardiac condition than had she not been employed in employment of that nature.”
The causative link between the development of her heart condition – the Broken Heart Syndrome – and her prior employment was accepted by the Commission, thus satisfying the s9A requirement (Workers compensation Act 1987) whereby the employment is a substantial contributing factor to the injury. The permanent impairment arising due to the heart injury was 20% whole person impairment, leading to an award of compensation of $48,940.
The employer unsuccessfully applied for leave to appeal, with the appeal rejected on the basis that it had no reasonable prospects of success:
What is significant in this case, are the comments of the expert cardiologists and the Commission’s acceptance and findings that the condition of Broken Heart Syndrome – Takotsubo cardiomyopathy – is a recognised and genuine consequence of the worker’s emotional distress.
